Our promise to you:
Guaranteed product quality, expert customer support.
 24x7 CUSTOMER SERVICE
24x7 CUSTOMER SERVICE
 CONTACT US TO ORDER
CONTACT US TO ORDER
Our promise to you:
Guaranteed product quality, expert customer support.
 24x7 CUSTOMER SERVICE
24x7 CUSTOMER SERVICE
 CONTACT US TO ORDER
CONTACT US TO ORDER
Chimeric antigen receptor (CAR) T cell therapy is a cellular therapy which redirects a patient's T cells to specifically target and destroy tumor cells. CARs are genetically engineered fusion proteins consisted of (1) an antigen recognition domain derived from a monoclonal antibody and (2) intracellular T cell signaling and costimulatory domains. Using CAR-T cells as a treatment for cancer has been most extensively investigated in patients with B cell malignancies, and early results have been encouraging. For example, CAR-T cell therapy has demonstrated complete response rates of 69%–90% in pediatric patients with relapsed or refractory acute lymphoblastic leukemia (ALL) in phase 1 trials. Moreover, the development of CAR-T cell therapy has now expanded beyond phase 1 trials and moved into phase 2 multi-site trials (NCT02435849 and NCT02228096).
CAR-T Cell Design
CARs are recombinant molecules which consist of antigen-binding variable regions of a monoclonal antibody. The activation and Co stimulatory domains of the T cell receptor complex are linked to these CARs. They are composed of an extracellular single-chain variable fragment (scFv) derived from an antibody, joined to a transmembrane domain and a hinge peptide, which is further linked to the intracellular T cell signaling domains of the T cell receptor.
In current clinical trials, CARs also include cytoplasmic signaling domains of T cell costimulatory receptors. In order to target a tumor-associated antigen in a human leukocyte antigen (HLA), independent manner T cell specificity is redirected by CARs. The extracellular domain provides CAR specificity for a tumor antigen. Designed intracellular domain helps to replicate the normal series of events by which T cells are activated. CAR-T cell therapies have the potential to kill targeted cancer cells that have evolved to escape immune surveillance through mechanisms such as proteasomal antigen processing or down-regulation of HLA expression, or in tumors that express negative co-stimulatory molecules that inhibit T cell activity (eg, PD-L1).
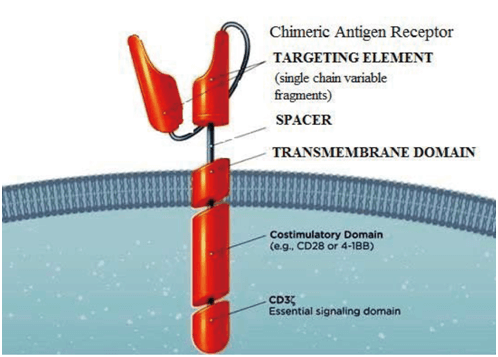
Figure 1. CAR-T Cell Design.
Production of CAR-T Cells
Currently, a major consideration for academic institutions and industry is how to scale out the production of CAR-T cells in an efficient, effective manner. The production of CAR-T cells requires several carefully performed steps, and quality control testing is performed throughout the entire protocol. Firstly, this process involves using leukapheresis to remove blood from the patient’s body, separate the leukocytes, and return the remainder of the blood to the circulation. After a sufficient number of leukocytes have been harvested, the leukapheresis product is enriched for T cells (Figure 2).
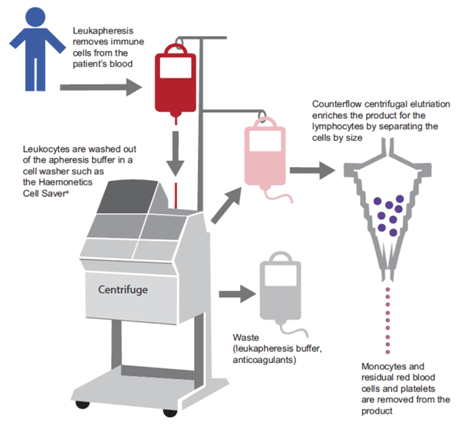
Figure 2. Production of CAR-T Cells.
During the activation process, the T cells are incubated with the viral vector encoding the CAR. After several days, the vector is washed out of the culture by dilution and/or medium exchange. The viral vector uses viral machinery to attach to the patient cells, and, upon entry into the cells, the vector introduces genetic material in the form of RNA. In the CAR-T cell therapy, this genetic material encodes the CAR. The RNA is reverse-transcribed into DNA and permanently integrates into the genome of the patient cells; therefore, CAR expression is maintained as the cells divide and are grown to large numbers in the bioreactor. Then, the CAR is transcribed and translated by the patient cells, and the CAR is expressed on the cell surface. Lentiviral vectors, which have a safer integration site profile than gammaretroviral vectors, are commonly used in clinical trials of CAR-T cell therapies, including CTL019.
Lentiviral Vectors: Transduction for CAR-T Cells
The major vectors for gene therapy in basic research and clinical study are viruses, because of the high transfer efficiency, the relatively short time needed to reach the clinically necessary numbers of cultured T cells and the availability of different viruses with different expression characteristics. Most viral systems can accommodate genes from helpful and interesting cells and can provide the viral structural enzymes and proteins to allow for the generation of vector-containing infectious viral particles. The virus vectors include retroviruses (including lentivirus), adenovirus and adeno-associated virus. Among them, the most popular tool for gene delivery is genetically engineered lentivirus. An advantage of lentiviral-derived vectors is that they retain the ability of lentiviruses to infect non-dividing cells, thus increasing their ability to transduce a wide variety of cells, including quiescent and difficult-to-transduce cells.
The viral vector is considered to be as a main raw material for the transduction of CAR into T cells of the CAR-T cell manufacturing process. The CAR-T cell product must be generated individually for each patient, but the vector by which CAR has been encoded can be made in large quantities and stored at -80℃ for 4 years. Frozen viral vectors are stable for about 9 years at this temperature. The vector to be used must be sterile because the final product (CAR-T cell) so produced can’t be sterilized by filtration or by any other sterility means. Use of a third generation minimal lentiviral vector, enhances safety. The minimum of two weeks is required for the batch manufacture of viral vector for cellular therapies. The major time is spent to grow adequate HEK293T cells in order to produce large quantities of replication-defective viral vector.
Plasmids are then transfected with the produced cells; the minimal lentiviral vector is produced as a result typically these plasmids are:
1) A packaging construct Gag/Pol packaging used to encode the structural (viral) protein (Gag) and enzyme (Pol);
2) A construct encoding appropriate envelope glycoprotein from a heterologous source, which results in pseudotyping of vector particle such as VSV-G;
3) A viral accessory expressing construct Rev; along with;
4) A plasmid vector which encodes the CAR construct and also other sequences essential for RNA, integration and ERT packaging.
Lentivirus vector usually comprises of three or four plasmid expression systems (Table 1).
Table 1. Plasmid expression.
| Transfer vector plasmid | Comprises the LTR, psi-sequence and therapeutic gene sequence. |
| Packaging vector plasmids | Comprises the elements required for virus packaging, such as genes coding for structural proteins, other genes (except the Env gene). This plasmid lacks the packaging signal owing to which the virus is rendered incapable of reproduction after it has infected host cell. |
| Envelope gene plasmid | Encodes the viral envelope proteins. |
Lentivirus Limitations
Insertional mutagenesis caused by the integration of vector DNA into host cells near an oncogene is a potential concern with all integrating vectors. However, lentiviral integration patterns favor sites away from cellular promoters, while γ-retroviral integration more frequently occurs near transcriptional start sites, suggesting that lentiviral vectors may carry a lower risk of mutagenesis. Risk for insertional mutagenesis also appears to be dependent on factors other than the vector system, such as the transgene that is encoded, the promoter, and the cell type or disease that is targeted. Oncogenic potential may be increased if replication competent lentiviruses (RCLs) are present in the vector products; however, current vector designs make the generation of RCLs highly unlikely. The FDA 2006 guidance considers lentiviral and retroviral vectors to be potentially oncogenic; therefore, vectors used in the clinic for CAR-T cell therapy are carefully tested for RCLs. In addition to testing for RCRs at multiple stages throughout the vector manufacturing process and the vector-modified cell product, the FDA also recommends that patients be followed for RCLs for up to 15 years to monitor any potential delayed adverse event related to these vectors.
References: